
Trauma
A mental, emotional, and physical response to an adverse experience.

Trauma is becoming a buzzword, but what does it mean? In this article, we’ll explore the spectrum of trauma and discuss how it relates to survivors of cancer and other rare diseases. We will also explore psychological or mind-based therapies for healing trauma as well as body-based therapies.
Though we don’t have diagnoses or firm understandings of all of the different kinds of trauma, we are beginning to understand that trauma exists on a spectrum. Not all traumatic events lead to diagnosable post-traumatic stress disorder, something we’ll explore in more depth later on. However, a person doesn’t need to have a diagnosis of post-traumatic stress disorder to acknowledge or begin healing from their trauma. There are many working definitions of trauma. We’ll explore some of them throughout this article.
The degree of trauma is dictated by the intensity of the traumatic event, the way the person experiences it, and the way the person processes it after the event has passed.
Below is an example of the spectrum of traumatic experiences and reactions a person may have with a cancer diagnosis.
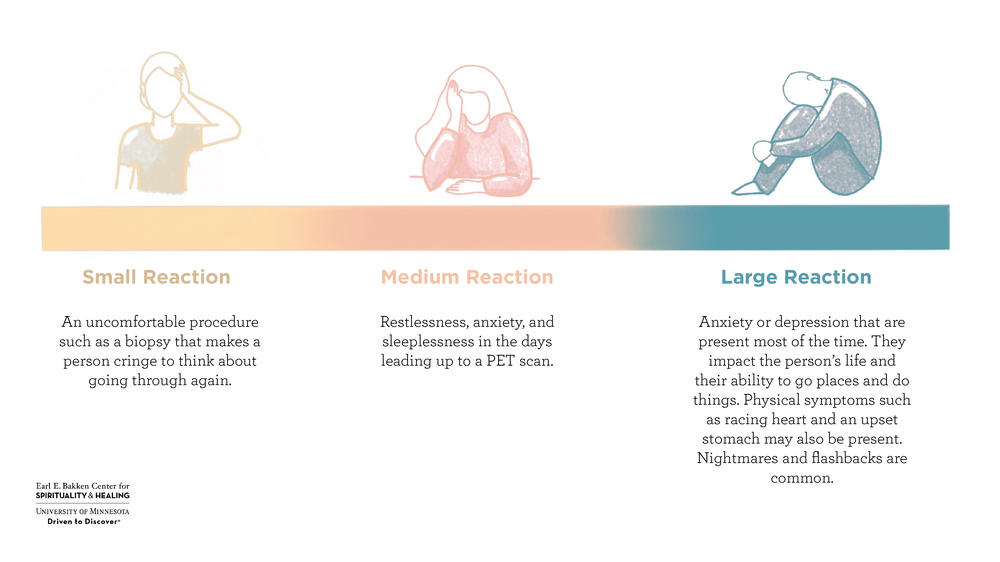
Traumatic events are the times when strong emotions cause physical reactions within us to keep us safe - the flight, fight, or freeze response. Examples include increased heart rate, blood shifting from internal organs to muscles- a response that prepares the body to run away from danger, but can leave a person unable to think clearly, digest food, or rest and heal.
Not all traumatic events lead to traumatic reactions, even though it would sometimes be healthier for us in the long run if they did.
It sometimes becomes second nature to interrupt our body's natural fear process by forcing ourselves to calm down. When the body isn’t allowed to experience fear or trauma, it becomes stored in the body in unhealthy ways, such as tension, pain, and anxiety.
Later on, any sensations that we associate with certain traumatic events can lead to traumatic reactions. Traumatic reactions are when we respond out of proportion to the present because of the past.
For example, our first experience receiving vaccinations as children can often be a traumatic event because of the needle poke. The traumatic reaction could range from slight trembling, to collapsing, or needing restraints when needles are involved even into adulthood.
The American Psychological Association defines trauma as “an emotional response to a terrible event like an accident, rape, or natural disaster. Immediately after the event, shock and denial are typical. Longer term reactions include unpredictable emotions, flashbacks, strained relationships, and even physical symptoms like headaches or nausea. While these feelings are normal, some people have difficulty moving on with their lives. [Mental health professionals] can help these individuals find constructive ways of managing their emotions.”
Just as everyone experiences trauma differently, everyone has different needs for healing from trauma. Unfortunately, healing from trauma is often a spiral process. Sometimes, a person may think they have processed their trauma and healed from it, only to have it bubble back up years later when something reminds the deepest part of their brain of the traumatic event. The brain then sounds the alarms that danger may be near. Learn more about Practices to Help Cope.
We'd like to thank the following contributors for their expertise and editing of this information.
Writing: Jacques Lerouge and Megan Voss
Design: Samuel Fedderly and Alissa Platzer