Diabetes

What is diabetes?
Diabetes Mellitis is a disease in which the body does not produce or properly use insulin, which affects how the body is able to use glucose for energy.
In order for cells to use glucose for energy, insulin must be present. In people with diabetes, the pancreas either produces little or no insulin (type 1), or the cells do not respond appropriately to the insulin that is produced (type 2 and gestational diabetes).
Glucose builds up in the blood, overflows into the urine, and passes out of the body in the urine. Thus, the body loses its main source of fuel.
The three main types of diabetes are:
- Type 1, also known as juvenile diabetes
- Type 2 diabetes
- Gestational diabetes (occurs in pregnant women during the pregnancy, but resolves after delivery)
What are the conventional treatments for diabetes?
When your physician diagnoses diabetes, it is likely that they will suggest, in addition to lifestyle changes, the following:
- Insulin (always in type 1 and sometimes in type 2)
- Monitoring blood sugar levels
- Oral medication (type 2)
The goal of all diabetic treatment is to normalize blood glucose (sugar) levels as much as possible, and to minimize the following long term complications of diabetes:
- Blood vessel damage that can lead to heart attack, stroke, limb loss, kidney damage, blindness, and other serious physical consequences
- Nerve damage, or neuropathy, resulting in loss of sensation
- Gastroparesis (delayed stomach emptying)
- Skin conditions
- Depression
While individuals with diabetes should check their blood sugar level multiple times per day, the best way to assess the overall level of glucose control is by taking a Hemoglobin A1C test. This provides an average of glucose levels over several months. National guidelines recommend that Hemoglobin A1C levels are measured four times per year. (The higher the Hemoglobin A1C, the more "uncontrolled" the diabetes.)
Routine monitoring of diabetes with a physician, and a coordinated care team, is very important in the proactive management of diabetes.
What are recommended lifestyle changes?
Lifestyle changes are critical in diabetes management, and are a routine and expected part of a conventional medical care plan. Some changes include:
- Healthy, low-fat, high-fiber, nutritious diet, minimizing simple and processed sugars. (Note that new research indicates that a plant-centered diet reduces risk of type 2 diabetes for young adults as they age.)
- Exercise
- Weight loss (if appropriate) or maintenance of a healthy weight
What are some integrative therapies to consider for diabetes?
Type 1 diabetes is not reversible or curable. With Type 2 diabetes, blood sugar can be normalized and managed without medication following adequate diet and exercise, although the ADA has not yet established criteria for diagnosis of actual cure. The following therapies and healing practices are therefore presented primarily as ways of managing type 1 and type 2 diabetes, optimizing function, and minimizing complications.
Traditional Chinese Medicine
The group of symptoms termed diabetes in conventional medicine has been treated for thousands of years with the system of Traditional Chinese Medicine (TCM). TCM looks at signs and symptoms in the context of the whole person. Specifically this system looks at patterns of disharmony, as well as patients' emotional and psychological responses.
Unlike conventional medicine, TCM does not focus on determining or manipulating the blood sugar levels, but rather individualizes a plan to restore balance and harmony, depending upon the nature of the diagnosed imbalance. The most commonly employed therapeutic methods in TCM include acupuncture, moxibustion, Chinese herbal medicine, diet therapy, mind/body exercises (Qigong and Tai Chi), and Tui Na (Chinese massage).
In 1997, the National Institutes of Health released a consensus statement saying that the use of acupuncture in the treatment of diabetes was classified as "effective, but further evidence required." It is important to acknowledge that the consensus statement referred to studies of acupuncture only, and not of the entire systemic approach.
Acupuncture has been shown to lower glucose levels and has been demonstrated to improve peripheral neuropathy and neuropathic pain, one of the most common complications of type 2 diabetes.
Many Chinese herbs and formulations have been used safely for millennia; however, good data on herb/drug interactions is limited. Additionally, the FDA does not regulate the preparation, prescription, or distribution of herbs. Therefore, it is important to work with a reliable and trustworthy source for herbal products. Heavy metal contamination is a concern for products grown in China. Some of the most commonly used herbs in diabetes include: Panax Ginseng, Momodica charantia, Lagenaria siceraria, and Psidium gnajava. These herbs appear to enhance how glucose is metabolized in the body.
Botanical Medicines and Supplements
The following supplements can be beneficial for those with diabetes. Typical doses for each botanical are indicated below. However, you should talk with your healthcare provider before adding botanicals to your health regimen and ask about the right dosage for you.
- Alpha-Lipoic Acid (ALA) is a strong antioxidant which improves glucose uptake and prevents glycosylation, a process in the body where sugars are inappropriately hooked onto proteins and fats. It may be good for prevention and to treat neuropathy. Doses range from 600-1,800mg/day. Thiamine should be supplemented when ALA is used in higher doses.
- Essential Fatty Acids can protect against the nerve and blood vessel damage from diabetes by increasing insulin secretion and lowering cholesterol levels. Take a dose of 1 Tbsp flaxseed oil and/or 1-4g of fish oil daily.
- Vitamin C acts as an antioxidant that improves insulin resistance and reduces free radical tissue damage. It is important for healthy immunity and wound healing. Dosage: 1-2 g/day.
- Ginkgo Biloba is an antioxidant and also acts to stabilize cell membranes. In diabetes, it is used primarily to help with peripheral circulation, but does carry some risk of bleeding. Dosage: 40-80 mg three times a day.
Conventional medications should not be discontinued in favor of herbs alone, unless they are weaned off over time, with close glucose monitoring. This requires a working team of an experienced physician and a knowledgeable TCM practitioner.
CAUTION: some herbs commonly used for weight loss may cause blood sugar levels to increase, including Coca seeds, Coffee seeds, Cola seeds, Guarana seeds, Mat'e leaves, and Ma huang.
Mind/Body Practices
Chronic stress elevates cortisol levels, which negatively impacts many different systems of the body. Stress increases the release of glucose from the liver and decreases insulin receptor sensitivity, making insulin work less effectively.
Stress management helps individuals be more effective in regulating their diet and exercising, which are both critical to diabetic management. Meditation, the Relaxation Response, Mindfulness-Based Stress Reduction (MBSR), and biofeedback are just a few of the practices that have been used to manage stress, and have positive impacts on the diabetic patient. See an example of the positive impact of Mindfulness-Based Stress Reduction.
How to use integrative therapies in your diabetes care
All of these approaches seek to optimize the body's ability to function. When integrating therapeutic approaches to diabetes, all patients must recognize the importance of careful monitoring of blood glucose levels, as well as monitoring for potential side effects, such as drug-herb interactions.
When new therapies and practices are added, ideally glucose levels will decrease or normalize, and prescription medications may need to be decreased in dose, or sometimes even eliminated. Therefore, reliable and regular self-testing of glucose levels, accurate recording/reporting, and frequent communication with your medical care team is critical.

Meditation Exercise
Meditation is one way to know yourself, and it has numerous other benefits. Listen to this audio to guide your meditation.
Sit comfortably with your feet on the floor.
Click the link below to start the audio, then close your eyes and listen. If you find your mind wandering gently bring it back and start again.

Tui Na (Therapeutic Massage) Video
Watch this video to see an example of tui na.
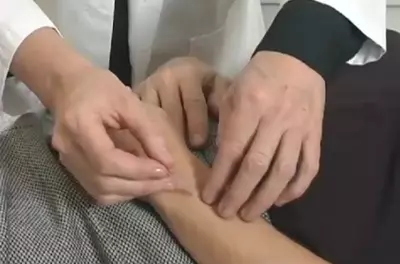
Acupuncture Video
Watch a video of an acupuncture treatment.

The Positive Impact of Mindfulness-Based Stress Reduction
Susie was a 27 year-old woman who had been diagnosed with Type 1 diabetes in her teens. She was very brittle, meaning that her glucose levels could swing very high or very low with minimal provocation. She commonly suffered from insulin reactions several times a week, when her glucose would drop so low, that she would have a seizure and/or lose consciousness before she could intervene and eat something. She would end up frequently being transported to the emergency room of the local hospital. Desperate to get better control of her life, she agreed to her physician's recommendation to enroll in an MBSR class. As she began a regular meditation practice, she became more aware of her body's symptoms when her glucose levels would begin to drop. She could then intervene before losing consciousness. Over time, she also became less brittle, with more stabilized and predictable glucose levels, and gained improved quality of life.
Books
Brand-Miller, J., MD (2004). The New Glucose Revolution Life Plan: Discover How to Make the Glycemic Index the Foundation for a Lifetime of Healthy Eating. Perseus Publishing.
Davis, B., Barnard, T. (2003). Defeating Diabetes. Healthy Living Publications.
Hammerly, M., MD. Diabetes: The New Integrative Approach : How to Combine the Best of Traditional and Alternative Therapies.
Mcdougall, J., MD (1991). The Mcdougall Program: 12 Days to Dynamic Health. Penguin Group.
Websites
The American Diabetes Association: http://www.diabetes.org
The Juvenile Diabetes Research Foundation: http://www.jdrf.org/
Healthy Humans has diabetes online programs: https://info.healthyhumans.com
Healthline Type 2 Diabetes Center: http://www.healthline.com/health/type-2-diabetes




